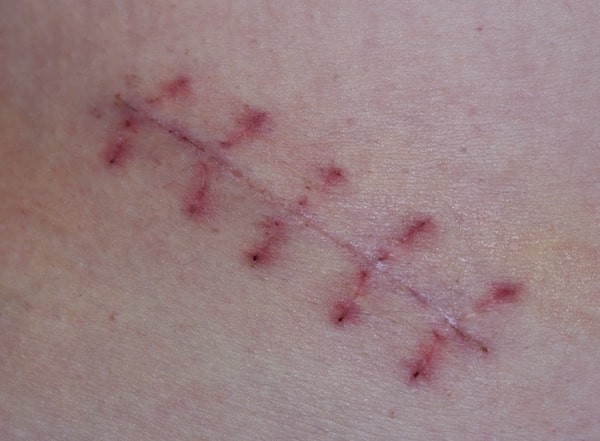
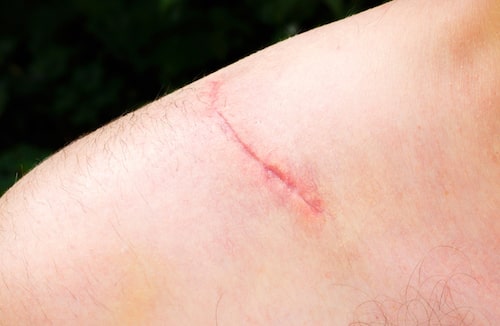
Scar tissue is often the result of an accident or a surgical operation and is also usually an unwelcome addition to the appearance of the body. Researchers at Stanford University have decoded the physical and chemical signals that work to trigger a certain type of skin cell to produce scars. In addition, the research team also have found a way to reprogram these cells in order to transform them into another type of cell that is able to regenerate intact tissues.
Research Team Results from Study on Mice
The team from Stanford University reported that mice that received the skin cell “trigger” were able to heal from wounds without the appearance of any scars. The mice regrew glands, hair, and other critical structures to the point that an image-classifying algorithm was not able to tell the difference between the area where the wound healed and the healthy part of the skin that was not damaged.
The research team says their next step is to try and achieve a similar type of skin regeneration in animals such as pigs (because they more closely resemble humans and have tighter skin). The Stanford team is optimistic these findings can lead to scar-free treatments becoming readily available in the future.
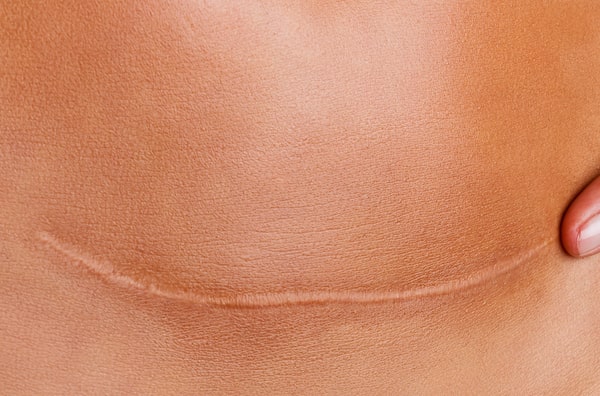
Scarless Wound Healing – A Goal that has been Years in the Making
It has been estimated that around 100-million patients gain scars each year after a surgical procedure. In addition, there are also millions of people that have some sort of injury or accident that results in a scar. The study by the team at Stanford represents the culmination of medical discoveries that date back to the 1970s.
In 1971, a Chicago pediatric surgeon discovered when he performed operations on fetal lambs, their wounds were able to heal without any type of scarring. Over the next two decades, the same healing ability was found in animals as varied as mice, sheep, pigs, and rats.
The early 1990s saw Michael Longaker, whose Stanford lab conducted the new research, working under Michael Harrison, a pediatric surgeon at the University of California, San Francisco. Harrison was performing surgeries on the unborn by removing a fetus from the uterus of the mother with the umbilical cord remaining intact. Once the medical issue or defect was addressed and resolved, the unborn child was returned to the womb. Once the baby was born, there would be some redness around the surgery site but there were no scars after the procedure.
Harrison asked Longaker to determine why this was happened and Longaker has spent the past three decades attempting to answer that question.
For a good portion of that time period, the research on the subject has almost always focused on stem cells AKA the cells that make all of the mini organs of the skin. Longaker incorporated the work of other scientists that studied fibroblasts (a cell located in connective tissue that produces collagen as well as other fibers) and were able to identify that there are different types of fibroblasts.
In 2015, his Stanford team amassed an inventory of the multiple types of fibroblasts that live on the skin located on the back of a mouse. The team found there was only one fibroblast subset (EPFs because they expressed a protein by the name of engrailed-1) that was responsible for the creation of most scar tissue. When this cell line was knocked out, the mice had less scarring along with a slower recovery period.
Their next task was to determine how the EPFs worked and if they could be turned off with a drug. If so, medical personnel might be able to stop scarring in humans. Longaker and his team have been working on this task for the past 3.5 years.
Scar-Free Healing and the Study of EPFs
The first step in the process was using fluorescent markers to track the origination of the EPFs. The research team learned scar-producing cells arise from another type of fibroblast, that regenerates healthy skin, and is “turned on” when the animal being studied was wounded. Longaker said the group hypothesized the trigger might be mechanical in nature such as the force of the skin being split apart.
The group then studied how fibroblasts respond to a number of different mechanical cues. When they were grown in soft substrates, they did not flip on engrailed-1. The group also studied the tension of wounds in mice and made the same discovery. They noticed that the application of more tension resulted in the production of a greater amount of a protein known as YAP.
In order to determine if YAP was the main chemical signal that started the scarring process, they blocked YAP with verteporfin (a YAP-disrupting chemical) and by genetically modifying the mice they were testing so they did not express YAP in their fibroblasts. In both cases, the cells that flooded into the wounds of the mice were not the EPFs that produced scars. Instead, they were the fibroblast that told the skin to regenerate instead of simply repairing the damaged area.
The mice that were treated using the YAP-blocker were able to recover their normal collagen structure as well as grow back their hair follicles and glands within a period of 30 days. In addition, their mechanical breaking strength was comparable to normal skin.
Scar-Free Healing – What the Future Holds
Even though the group led by Longaker was able to show the return of some skin structures, it was not a complete list so more work will need to be performed by the research team. The additional research is needed to see if YAP-blockers are able to turn on all of the necessary signals to regrow all of the needed elements for healthy skin to be able to function.